Senior dog presents with a gradual decline in mobility, no mechanism of injury but more generalized weakness especially in the pelvic limbs.
Veterinary evaluation without rads- diagnosis osteoarthritis, prescribed Librela and after six months no significant improvement. Librela had been discontinued and the senior dog did have some urinary incontinence and history of a UTI that occurred after Librela. Another feature was she lost of some of her fur along her back and she seemed to have some cognitive decline and more anxiety. She did have a history of skin issues prior but they had resolved with a fresh food diet and supplementation.
Given there was no significant improvement with medication over six months, a decline in mobility and an increase in anxiety, and her pet parents were wondering if it’s “time” and trying canine rehab as a last resort.
The above is a brief presentation of a recent new assessment. Sadly, I see these cases a lot. And let me preface this with I’m not a veterinarian, I am a licensed physiotherapist with a diploma in canine rehab. This isn’t about my opinions on Librela. It’s the clue it leaves us with.
Librela is designed to reduce pain signal in joints with osteoarthritis (OA) … So, why didn’t it work? What could that mean?

Presentation (What I saw)…
I have seen several senior dogs present this way. A diagnosis of OA but continuing to have declining mobility despite the prescribed rest and medication. They come in, head and tail low, walking anxiously around the clinic often at a pace (unnatural gait), they sometimes trip a little over a front paw and their back legs are visibly weak and sometimes they look sore in one of their back legs.

Sky pre-treatment
An interesting and relevant note about pacing. It’s not natural.
Pacing is when the dog’s front and rear leg on the same side moves in the same direction. Sometimes they’re trying to match your speed while on leash, but it is also observed in dogs that have back pain. It requires less rotation of the spine than trotting and is therefore easier or more comfortable for the dog to do.
The dogs often have minimal if any “upper motor neuron” (UMN) deficits. These are reflexes like conscious proprioception (knuckling correction), withdrawal (toe pinch), and deep tendon reflexes (tested with reflex hammer).
On palpation (touch) things get super interesting!
Often there are a lot of short and tight muscles, generalized muscle atrophy, the presence of “myofascial trigger points” (MTrP) which are painful “knots” in the muscles that have a twitch response.
MPS is a chronic pain condition that involves active MTrPs.

Back to our senior dogs…If you feel along the midline of their backs, their spinous processes (boney bumps down the centre of their back – spine) are more prominent. Maybe your dog is similar…? And there’s atrophy of the epaxial muscles that run along either side the spine.
The spine is usually hypomobile (stiff) when testing each vertebrae and there are areas with excessive fasciculations (twitching) often accompanied by pain (I.e. dogs’ back drops away during palpation or they express they don’t want to be touched there).
My conclusion or “pathofunctional diagnosis” of this senior pup…
Looking at the presenting dog’s whole body, how she moved and felt, plus her history, I believe her decline in mobility was related to back pain, spinal stiffness which may or may not be related to arthritis in the spine (remember, no x-rays, just spinal stiffness) and the presence of MTrP which we know are painful and inflammatory.
This would also explain why the Librela didn’t work.

Stay with me here because there is more evidence!
The potential link between trigger points and anxiety…
amygdala human brain
As I previously mentioned MPS is a well known cause of chronic pain in people. Chronic pain is associated with something called “central sensitization”. In simplest terms, the central nervous system changes and becomes over-sensitized to pain. Long term MTrP can produce these changes. What’s even more fascinating is that the amygdala (part of the brain) has been observed to have abnormal activity in response to pain associated with MTPs (https://doi.org/10.3389/fvets.2025.1488801)!
This is interesting because the amygdala is the part of the brain associated with processing fear and anxiety. Remember I mentioned these dogs I’ve seen present this way generally seem to be more anxious or their pet parents report concerns about anxiety and cognitive changes. Keep read, there’s more!
OA joints may not be related to trigger points in associated muscles!…
A recent canine study showed that the presence of MTPs and joints affected by arthritis were not correlated (you read correctly, not related). However, age was. As the dog aged, there was a higher presence of MTrP with the most in a muscle called “longissimus thoracicae” which is one one of the epaxial muscles I mentioned. The second most prevalent muscle was the quadricep femurs on the front of the thigh going from the pelvis crossing the knee joint and attaching to the lower leg bone (tibia) (https://doi.org/10.3389/fvets.2025.1488801).
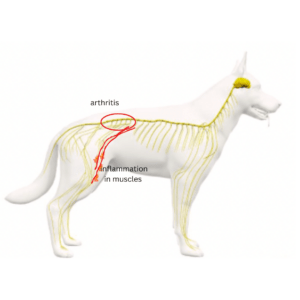
Spinal OA and inflamed innervated muscles
This is the “big aha”…
Studies on humans have shown that there are higher inflammatory markers in muscles with MTrP (https://doi.org/10.1016/j.berh.2024.101944).
And the spine arthritis connection… there’s evidence that there are higher levels of inflammatory markers in muscles supplied by nerves connected to segments of the spine that have arthritis and not muscles connected to other parts of the spine (https://doi.org/10.1016/j.exger.2021.111311)!
Boom!
OK, I may have gotten a little too excited about this, but I believe it’s so important when it comes to helping our dogs move and feel better. Are you looking in the right place? Not everything is solved with a pill.
Let’s bring all together…
I recognize this might be a lot to wrap your head around so let’s see if I can summarize it for you. Here is what we know about the presenting dog and similar past cases I’ve seen:
- Senior dog, decline in mobility and an increase in hind weakness
- Pet parents reported they didn’t think Librela helped and felt their dogs were more anxious
- Range of motion was guarded and there were soft tissue restrictions and MTrPs, and spinal stiffness
- Gait changes including pacing are observed as well as changes in the coat
And the research says…
- The amygdala is associated with the fight or flight response and in dogs with MTrps abnormal activity in the amygdala was observed
- A correlation between chronic pain and MTrP which has not been studied with dogs but has in humans
- MTrP are inflammatory
- There is a correlation between segments of the spine with OA and the muscles they innervate having higher levels of inflammatory markers then surrounding muscles
- MTrP are painful and associated with MPS which is one of the most common sources of chronic pain in people

Buddy post treatment 💙
Treating the spine and the soft tissue is gold
When I’ve treated the soft tissue restrictions, MTPs, the spine including the cervical spine (this is a different conversation but relates to both degenerative changes and compensation), these dogs have improved dramatically in terms of pain and mobility.
Now can I “BOOM?!?
What does all this mean for your dog?




I hope this made you as excited as it made me! Even more, I hope you feel more informed and ultimately this helps your dog move and feel better.
If you need help, reach out!
I am available:
And have:
You can help your dog move better and feel better!
PS – if you found this helpful, please share it and help dogs globally improve their mobility and decrease their pain
References
Broadhurst, M., Dr., & Angus, A., Dr. (2019). A Clinicians Guide to Myofascial Pain in the Canine Patient (1st ed.). Amazon.ca.
Duarte FCK, Hurtig M, Clark A, Brown S, Simpson J, Srbely J. Experimentally induced spine osteoarthritis in rats leads to neurogenic inflammation within neurosegmentally linked myotomes. Exp Gerontol. 2021 Jul 1;149:111311. doi: 10.1016/j.exger.2021.111311. Epub 2021 Mar 17. PMID: 33744392.
Formenton MR, Fantoni DT, Gauthier L, Cachon T, Yeng LT, Portier K. Prevalence and location of myofascial trigger points in dogs with osteoarthritis. Front Vet Sci. 2025 Jan 15;12:1488801. doi: 10.3389/fvets.2025.1488801. PMID: 39886026; PMCID: PMC11776090.
Lam C, Francio VT, Gustafson K, Carroll M, York A, Chadwick AL. Myofascial pain – A major player in musculoskeletal pain. Best Pract Res Clin Rheumatol. 2024 Mar;38(1):101944. doi: 10.1016/j.berh.2024.101944. Epub 2024 Apr 21. PMID: 38644073.
Wall R. Introduction to myofascial trigger points in dogs. Top Companion Anim Med. 2014 Jun;29(2):43-8. doi: 10.1053/j.tcam.2013.11.001. Epub 2014 Feb 12. PMID: 25454375.








